What is a Corneal Transplant?
A corneal transplant is a surgical procedure that replaces all or part of your damaged cornea with donor corneal tissue. Corneal transplants can be categorized as “full thickness” or “back layer.” The goal is to replace damaged or diseased cornea tissue that is impacting the patient’s vision beyond what can be corrected with eyeglasses or contact lenses.
Corneal transplants are very common in the United States; about 40,000 are performed each year. While success rates may vary due to pre-existing conditions in your eye, technological advancements have increased your chance of success. Approximately 90% of corneal transplants are successful, and the new cornea will stay healthy for an average of 10 years. In the unlikely event that your surgery is not successful, or if your cornea does become cloudy again, you can always receive another transplant.
What To Expect During a Cornea Transplant
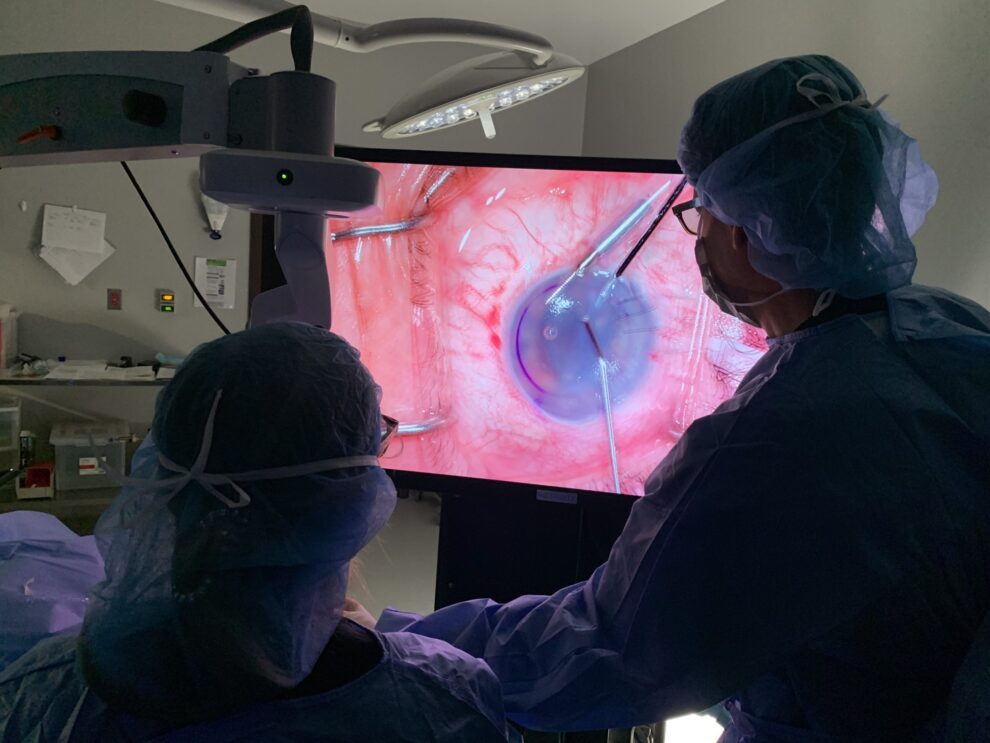
During the corneal transplant surgery, Dr. Schultze or Dr. Eden will remove an eight-millimeter central portion of the cloudy or damaged cornea and replace it with a new, clear one. Your new cornea will often come from an eye bank after being screened for suitability and infectious diseases.
Your surgeon will place the brand new cornea in the opening left from removing the old cornea and secure it in place with a very fine suture. These tiny sutures will remain in your eye for a few months while the eye heals, and then will be removed easily and gradually during visits to our office.
Post Cornea Transplant
Your surgeon will prescribe you eye drops to use after surgery to help your eye heal and to prevent infection. Your vision will be blurry at first due to stitches and post-operative swelling, but most people are able to return to work and daily life about a week after surgery. Full visual recovery can take up to a year, and it is vital that patients take their medication as directed, keep follow-up appointments and pay close attention to any increased redness, discharge, sensitivity to light, pain or blurring. This can be an indication of transplant rejection and should be reported to our office immediately so that we may be able to reverse the condition.
What are the Alternatives to a Corneal Transplant?
Phototherapeutic Keratectomy (PTK)
Phototherapeutic keratectomy (PTK) is one of the latest advances in eye care. It allows patients with corneal dystrophies, corneal scars, and certain corneal infections to avoid a corneal transplant.
These procedures combine the precision of the excimer laser (the same laser used in LASIK procedures) with the control of a computer, allowing Dr. Schultze or Dr. Eden to vaporize microscopically thin layers of diseased corneal tissue and etch away the surface irregularities associated with various corneal dystrophies and scarring. PTK surgery removes the epithelium, along with some of the underlying corneal stroma. This new procedure allows the patient to keep his or her cornea, and new tissue will grow over the surface that has been smoothed.
The primary goal of a PTK is to produce a smoother and clearer cornea. You may still need to wear glasses to attain your best vision, but PTK should make dramatic improvement.
Deep Anterior Lamellar Keratoplasty (DALK)
Deep Anterior Lamellar Keratoplasty (DALK) is an additional newer method of corneal transplantation. It only replaces the superficial layers of the cornea, so there is less risk of damage to the eye. You are a good candidate if you have a disease that only affects the outermost layers of the cornea, like keratoconus. Because this procedure is extremely technical, the success rate is approximately 75%. Fortunately, if the cornea does not divide optimally at the time of the procedure, a full-thickness keratoplasty remains an option to rehabilitate vision. The advantages to DALK include greater structural integrity of the eye and decreased the chance of rejection.
EK (Endothelial Keratoplasty)
Endothelial Keratoplasty (EK), also known as Descemet Stripping Automated Endothelial Keratoplasty (DSAEK), is a newer method of corneal transplantation and only involves replacing some of the posterior or inner layers of the cornea, instead of its full thickness as in standard corneal transplantation. For this reason, if your disease affects the full thickness of the cornea, you are not a candidate for EK.
Center For Eye Care Excellence doctors have been pioneers in the field of endothelial keratoplasty. They were the first surgeons to perform the procedure in the state of New York in 2003 and have been extremely successful. Drs. Schultze and Eden are the recognized leaders in Northeastern New York in advanced techniques of corneal transplant surgery and are acknowledged around the world for their research and achievements.
Benefits of an Endothelial Keratoplasty
While EK is a relatively new surgery and therefore hasn’t been studied as thoroughly as the standard procedure, there are many advantages. Compared to the standard transplant procedure, your surgeon can make a smaller incision in the eye so fewer stitches are needed. Your recovery is drastically shortened with the eye healing in 3-6 months, as opposed to a year. Your eye will have less chance of injury during surgery, and with fewer stitches, there is less chance of infection.Schedule Your Consultation Today!
Descemet Membrane Endothelial Keratoplasty (DMEK)
A Descemet membrane endothelial keratoplasty (DMEK) is very similar to DSAEK, except that the implanted donor tissue does not include any stromal tissue. A DMEK is an exciting option to treat decreased vision and swollen cloud corneas and it is a pure replacement of endothelium. There are three generations in the evolution of corneal transplantation and DMEK is the third and newest, but the surgeons of Center For Eye Care Excellence have been performing this surgery for three years and were some of the first in the Northeast to do so. DMEK is the most anatomical repair of the three generations of corneal transplantation with just one cell layer and a thin membrane, all of which are only 15 to 20 microns thick.
What to expect during DMEK procedure
During DMEK surgery, the diseased innermost layer of the cornea is removed and the thin layer from a healthy donor cornea is put in its place. The transplant is then held in place by only an air bubble. Patients will be required to lay flat on their backs with their faces directed upwards immediately after surgery to float the bubble into place. DMEK has been shown to offer patients the best chance to see 20/25 and resume their daily activities quickly.